Candidemia Reduction Estimator
Calculate Potential Reduction
Estimate how much implementing specific infection prevention measures could reduce candidemia rates in your unit.
IPC Measures to Implement
Estimated Impact
Enter your current candidemia rate and select IPC measures to see potential reduction.
Key Takeaways
- Candidemia and disseminated Candida infections carry high mortality, especially in ICU patients.
- Effective infection prevention and control (IPC) hinges on hand hygiene, catheter care, environmental cleaning, and antifungal stewardship.
- Surveillance data together with rapid lab diagnostics enable early outbreak detection.
- Bundled IPC interventions can cut Candida bloodstream infection rates by 30‑50%.
- Regular staff training and audit feedback sustain long‑term compliance.
When a patient develops Candidemia is a bloodstream infection caused by Candida species, most often Candida albicans, with a reported mortality of 30‑45% in intensive care units, rapid identification and containment are critical. infection prevention measures aren’t an afterthought - they’re the frontline defense that turns a potential outbreak into a manageable event.
Why Candidemia and Disseminated Candida Infections Matter
These invasive fungal infections account for roughly 8‑10% of all hospital‑acquired bloodstream infections in high‑income countries. The burden is amplified in patients with central venous catheters, neutropenia, or recent broad‑spectrum antibiotic exposure. Mortality rates climb above 40% for disseminated disease, where Candida spreads to organs such as the kidneys, brain, or eyes. The economic impact includes longer ICU stays, higher drug costs, and increased use of isolation resources.
Core Principles of Infection Prevention and Control
IPC for Candida infections rests on three pillars: (1) interrupting transmission pathways, (2) reducing host susceptibility, and (3) ensuring optimal antifungal use. Each pillar maps to concrete actions that can be audited and reported.
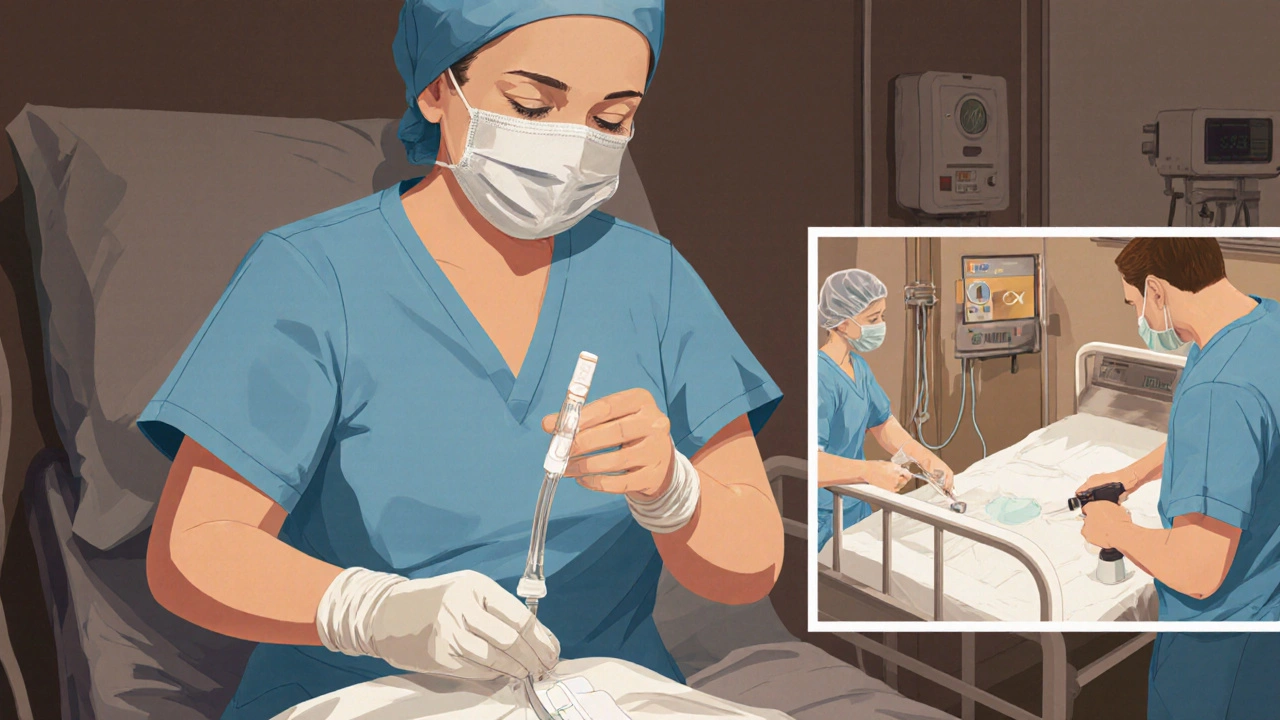
Hand Hygiene and Contact Precautions
Hand hygiene remains the single most effective measure. Studies show a 25‑35% drop in Candida bloodstream infections after achieving >80% compliance with alcohol‑based hand rubs. When handling patients with confirmed or suspected candidemia, add contact precautions-gloves and gowns-to prevent cross‑contamination from skin colonization sites.
Central Line Management
More than 70% of candidemia cases are linked to central venous catheters (CVCs). The Central Venous Catheter is a medical device inserted into a large vein for fluid, medication, or nutrition delivery; it provides a direct conduit for microbes into the bloodstream must be managed with a sterile insertion bundle, daily necessity assessment, and prompt removal when no longer essential. A “maintenance bundle” that includes chlorhexidine‑impregnated dressings and routine hub disinfection with >70% isopropanol can cut catheter‑related candidemia by up to 50%.
Environmental Cleaning and Disinfection
Candida can persist on surfaces, especially in humid environments. Environmental Cleaning is the systematic removal of microbial contaminants from patient‑care areas using approved disinfectants and validated protocols should focus on high‑touch surfaces, infusion pumps, and ventilator circuits. In units with Candida auris is an emerging, multidrug‑resistant yeast notorious for persisting on bedside rails and medical equipment, the CDC recommends using sporicidal agents (e.g., chlorine‑based solutions) as part of daily cleaning.

Antifungal Stewardship and Surveillance
Antifungal stewardship aligns prescription practices with susceptibility data to limit resistance. A stewardship program that tracks azole and echinocandin use, coupled with real‑time susceptibility dashboards, can reduce inappropriate antifungal therapy by 30% and lower emergence of resistant strains.
Surveillance is the eyes of the program. Weekly incidence reports of Disseminated Candida Infection is a systemic spread of Candida beyond the bloodstream, often involving organs such as the liver, spleen, or eyes; it signals advanced disease and higher mortality allow infection control teams to spot clusters early. Many hospitals adopt the CDC’s NHSN BSI reporting module, which captures organism, source, and patient risk factors.
Outbreak Investigation Workflow
- Confirm case definition - lab‑confirmed candidemia plus clinical criteria.
- Generate a line‑list of affected patients, noting CVC presence, location, and antifungal exposure.
- Conduct a point‑prevalence environmental culture focusing on sinks, ventilator surfaces, and medication carts.
- Review hand‑ hygiene audit data and compliance trends over the prior 30 days.
- Implement immediate control measures: reinforce hand hygiene, isolate affected patients, and replace potentially contaminated CVC kits.
- Report findings to hospital leadership and update the IPC bundle based on identified gaps.
Implementing an IPC Bundle: A Practical Checklist
| Measure | Target Population | Expected Reduction (%) | Evidence Source |
|---|---|---|---|
| Alcohol‑based hand rub compliance >80% | All HCWs | 25‑35 | JAMA 2022; multicenter trial |
| Daily CVC necessity assessment | ICU patients | 30‑45 | Infection Control Hum. 2021 |
| Chlorhexidine‑impregnated dressings | CVC sites | 40‑50 | Clinical Infect. Dis. 2020 |
| Environmental cleaning with sporicidal agents | Units with C. auris | 35‑40 | CDC 2023 Guidance |
| Antifungal stewardship audit | Prescribing clinicians | 20‑30 | Antimicrob. Agents Chemother. 2021 |
Embedding this bundle into daily workflow requires a champion - often the infection control nurse - who runs weekly compliance dashboards, provides real‑time feedback, and celebrates milestones. Data‑driven recognition keeps the team motivated.
Frequently Asked Questions
How quickly should a central line be removed after a positive Candida blood culture?
Guidelines recommend removal within 24‑48hours if the line is not indispensable for life‑support. Early removal reduces mortality by up to 15% and shortens ICU stay.
Is contact isolation necessary for all patients with candidemia?
Contact precautions are advised for patients colonized with multidrug‑resistant species like Candida auris. For common Candida albicans infections, strict hand hygiene is usually sufficient unless there’s an outbreak.
What role does environmental surveillance play in preventing Candida outbreaks?
Targeted environmental cultures identify hidden reservoirs such as sink drains or reusable equipment. Findings guide enhanced cleaning protocols and can prevent up to 40% of transmission events.
How can antimicrobial stewardship programs address antifungal resistance?
Stewardship teams monitor azole and echinocandin usage, enforce de‑escalation based on susceptibility, and provide decision‑support alerts. This approach curbs unnecessary exposure and slows resistance emergence.
What are the most common risk factors for disseminated Candida infection?
Key risks include prolonged neutropenia, recent abdominal surgery, total parenteral nutrition, and colonization with Candida in the gastrointestinal tract. Early identification of these factors triggers pre‑emptive IPC measures.
By marrying rigorous hand hygiene, meticulous catheter care, targeted environmental cleaning, and a robust antifungal stewardship framework, hospitals can dramatically lower the incidence of candidemia and its dreaded disseminated form. The payoff isn’t just numbers on a report - it’s fewer lives lost and a healthier workforce.




16 Comments
Val Vaden-13 October 2025
Looks like a fancy calculator, but real wards still need basic hygiene 😒
lalitha vadlamani-14 October 2025
While the authors present an appealing interface, the moral imperative to prioritize patient safety cannot be reduced to a widget. The emphasis on hand‑hygiene compliance is commendable, yet it must be backed by rigorous auditing. Moreover, the tone of the article borders on complacency, overlooking the ethical duty to educate frontline staff continuously.
kirk lapan-15 October 2025
The manuscript attempts to distill a massive body of infection control literature into a clickable calculator.
While the concept is laudable, the real challenge lies in translating those percentages into bedside practice.
For instance, the reported 40‑50% reduction from chlorhexidine dressings hinges on perfect compliance, which is rarely achieved outside of study settings.
Moreover, the tool assumes additive effects of interventions, ignoring potential overlap that can blunt the cumulative impact.
Hand hygiene compliance >80% is repeatedly cited, yet many units struggle to sustain even 60% without continuous auditing.
Central line assessment bundles are effective, but they require daily multidisciplinary rounds that many hospitals cannot staff.
Environmental cleaning for C. auris is critical, but the recommendation to use sporicidal agents can damage equipment if not carefully managed.
Antifungal stewardship audits sound beneficial, but they depend on a robust microbiology reporting infrastructure that many community hospitals lack.
The calculator also overlooks patient‑specific risk factors such as neutropenia duration or prior azole exposure.
In practice, a one‑size‑fits‑all reduction estimate can give false reassurance to administrators.
The authors could improve the tool by incorporating a risk‑adjusted scoring system.
Including a feedback loop where unit‑level data refine the percentages would make the estimator more dynamic.
A discussion of cost‑effectiveness for each measure would also enhance its utility for budget‑constrained facilities.
Finally, the manuscript would benefit from a clearer description of the validation cohort used to derive those reductions.
In its current form, the calculator is a nice educational adjunct but falls short of being a decision‑support instrument for frontline clinicians.
Landmark Apostolic Church-15 October 2025
Interesting points, but we must remember that infection control is as much about culture as it is about tech. A calculator can’t replace daily conversations on the unit floor.
Matthew Moss-16 October 2025
Our hospitals must lead the world; these guidelines are a step toward American excellence. Anything less would be a betrayal of our medical heritage.
Antonio Estrada-17 October 2025
Agreed, the focus on adherence is key, and we can share best practices across institutions. Mutual support will amplify the gains.
Andy Jones-17 October 2025
Oh great, another spreadsheet to fill out-just what the ICU needed.
Kevin Huckaby-18 October 2025
😂 Honestly, if I saw a nurse spend ten minutes on a calculator I’d hand them a coffee instead.
Brandon McInnis-19 October 2025
The checklist format is useful, but implementation fatigue can undermine its benefits. Keeping the team motivated is half the battle.
Todd Peeples-19 October 2025
From a systems‑engineering perspective, the modularity of the IPC bundle facilitates iterative refinement and real‑time feedback loops, thereby optimizing both efficacy and resource allocation.
Chris Smith-20 October 2025
nice try but looks like a marketing gimmick
Leonard Greenhall-21 October 2025
data shows overlapping interventions reduce marginal gains; tool should reflect diminishing returns
Abigail Brown-21 October 2025
Wow, this could really change the game! Imagine fewer families grieving because of faster interventions. The hope is palpable.
Crystal Slininger-22 October 2025
I suspect the pharma lobby is behind the emphasis on antifungal stewardship-they want us to buy more expensive drugs.
Sumeet Kumar-23 October 2025
👍 Let's keep pushing these measures, every percent counts!
Maribeth Cory-24 October 2025
Absolutely, collaboration across disciplines will turn these numbers into real‑life savings.